New Study Identifies Challenges for COVID-19 Vaccine Adoption
In-Depth Interviews Identify Key Obstacles to Overcome for Broad COVID-19 Vaccine Adoption
STUDY HIGHLIGHTS:
- Half of participants say they are likely to take the COVID-19 vaccine as soon as it is available
- Safety and minimizing side effects are the most important factors driving decisions
- Two thirds of those not likely to take the vaccine doubt its safety
- Women are more often the gatekeepers for households and are less likely to take the vaccine than men
- Over one third of doctors and nurses are not yet supportive of taking a COVID-19 vaccine
- Some do not consider their doctor’s recommendation important and are leery of new vaccines
- President-elect Joe Biden’s victory had a net positive impact on vaccination adoption
Several pharmaceutical companies have made significant progress in the development of a COVID-19 vaccine, and are planning distribution for high priority segments of the U.S. population beginning in the next few weeks. While this is exciting news, it will take some time before a vaccine will be available for the general public – optimistically by April to June, 2021, according to Dr. Anthony Fauci.
One of the questions that remains is “will enough of us choose to take the vaccine?” Recent surveys indicate about half of Americans plan not to take the vaccine when it becomes available. Last month, Dr. Fauci said, “We know what the efficacy of the vaccines are, but its effectiveness will depend on how many people take the vaccine.”
We wanted to understand the perspective of both the medical community and the general public to identify a path to a higher vaccine adoption rate. We conducted a series of one-on-one, in-depth phone interviews (average length of 30 minutes) with doctors, nurses, and members of the general public to better understand what needs to happen in order for Americans to feel comfortable choosing to get vaccinated.
The 40 participants in our study included 17 individuals from the medical community (11 doctors, six nurses) and 23 members of the general public. The findings from this small study should be considered directional as this was not a large population study, and we prioritized deeper, live interactions over sample size. Participants constituted a diverse representation of American society, across gender, race, income, geography, employment status, level of education, political affiliation, and other demographic factors.
We are sharing the findings from our research in the hope that health experts use this information to help prioritize what areas to focus on and to help determine the most effective messages to maximize vaccination adoption. More research needs to be done, but we hope these results will be of value in the national effort to vaccinate the population.
Key Findings from our COVID-19 Vaccine Study:
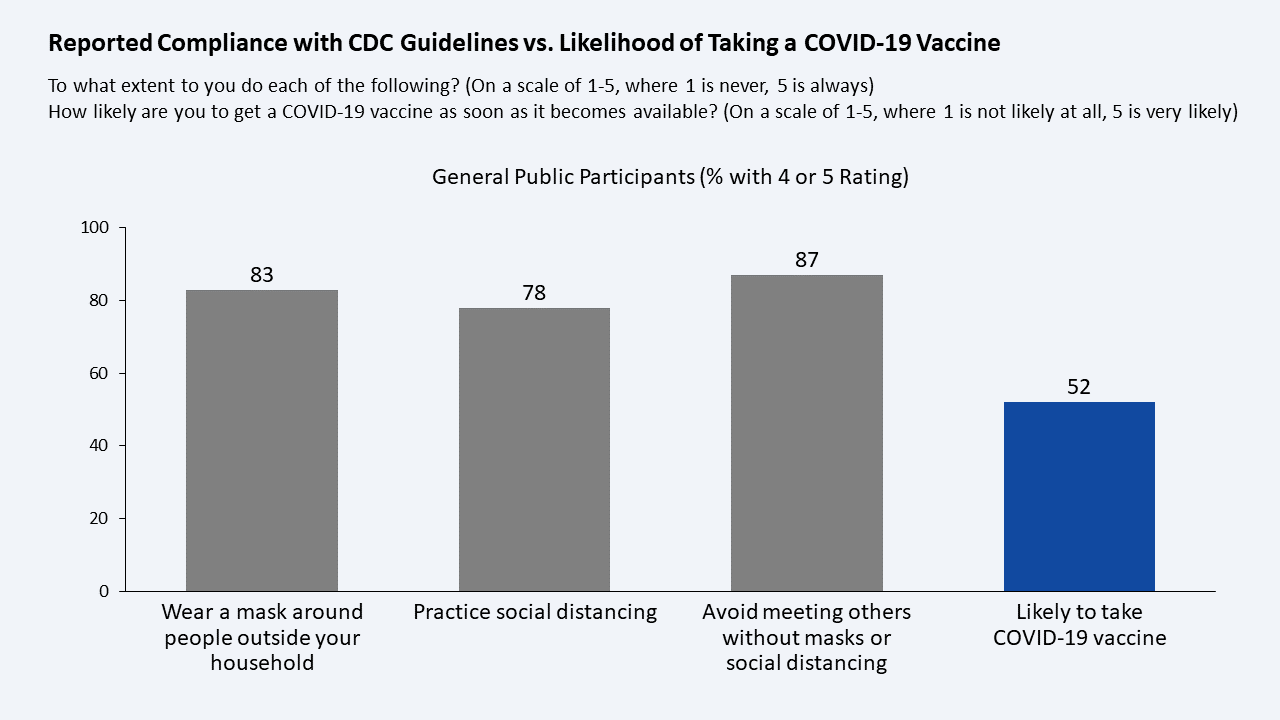
Low Expected Adoption Rates:
Finding: 52 percent of the general public participants indicated that they are likely to take the vaccine as soon as it becomes available to them. This number is in line with recent surveys that have the figure in the 40 to 60 percent range. Participants reported high compliance rates with CDC guidelines for wearing a mask around people outside the household (83 percent), practicing social distancing (78 percent), and avoiding meeting others without masks or social distancing (87 percent). These compliance rates for preventative measures are much higher than the 52 percent vaccine adoption rate.
Why This is Important: In order for the country to move past the pandemic and into a closer-to-normal day-to-day life, the World Health Organization estimates that 65 to 75 percent of the population – well over 200 million Americans – need to have antibodies either by means of a vaccine or through recovery from the virus (which still has an uncertain level of immunity). At this roughly 70 percent level, the spread of the virus is expected to slow down to the point that we will offer herd immunity, so that, as in the case of viruses such as polio and smallpox, COVID-19 will be decimated.
Implications: We have significant progress to make to close the 20 percent adoption gap required for herd immunity. The virus will not be vanquished until enough people become immune. It is critical for health leaders and policymakers to make significant strides in public trust and support of the vaccine.
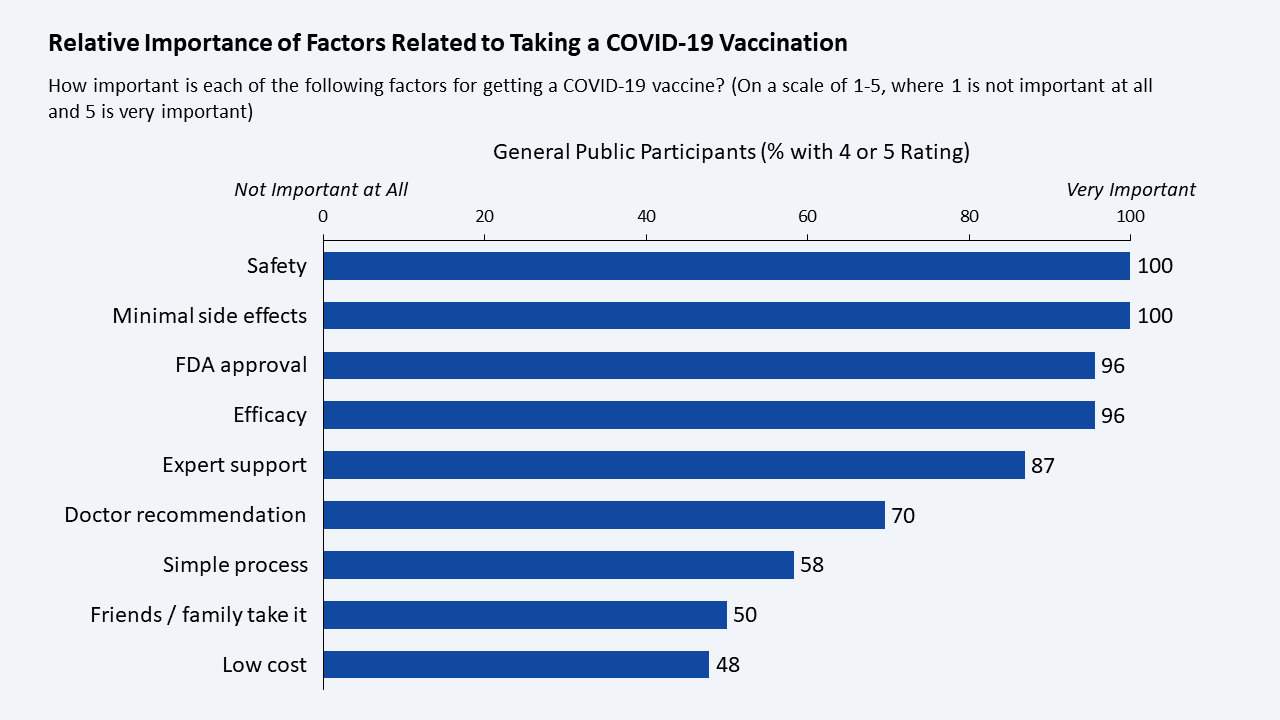
Safety First:
Finding: Overall, the most important factors for taking a COVID-19 vaccine are safety, minimal side effects, FDA approval, efficacy, and public support from medical experts. M. (participant names concealed to preserve anonymity), a merchandiser from Columbus, Ohio, explained, “I need to know that it’s safe before I get it. And, it has to be, without a doubt, effective.”
Why This is Important: Over 85 percent of study participants indicated that these five factors are of paramount importance. These factors were generally viewed as the bare minimum criteria for getting the vaccine. Other factors, including affordability and the participation of friends and family, were viewed as much less important.
Implications: These five areas should be considered “must haves.” Americans need to see clear and compelling evidence in these five “must have” areas. The length of the testing period, the size of the population tested, and the level of diversity of testing groups (e.g., by gender, race, risk level, etc.) were commonly mentioned throughout our interviews as critical to gaining the public’s confidence.
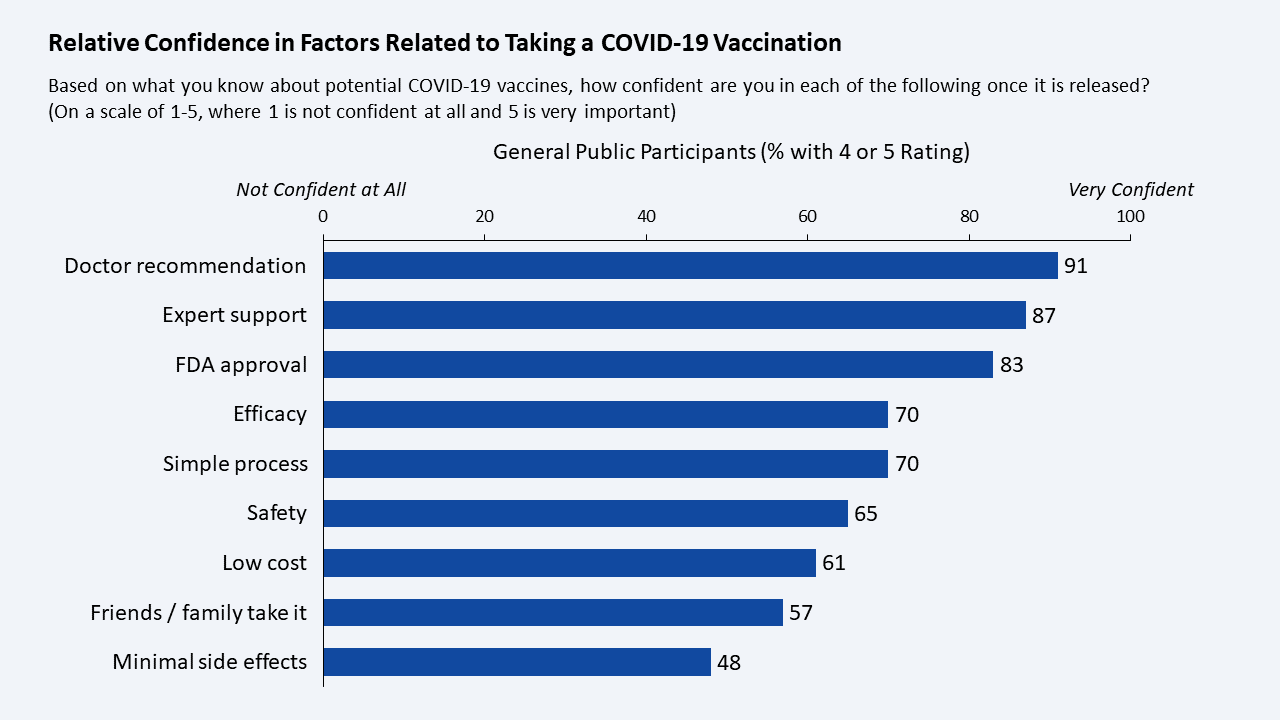
Big Confidence Gap:
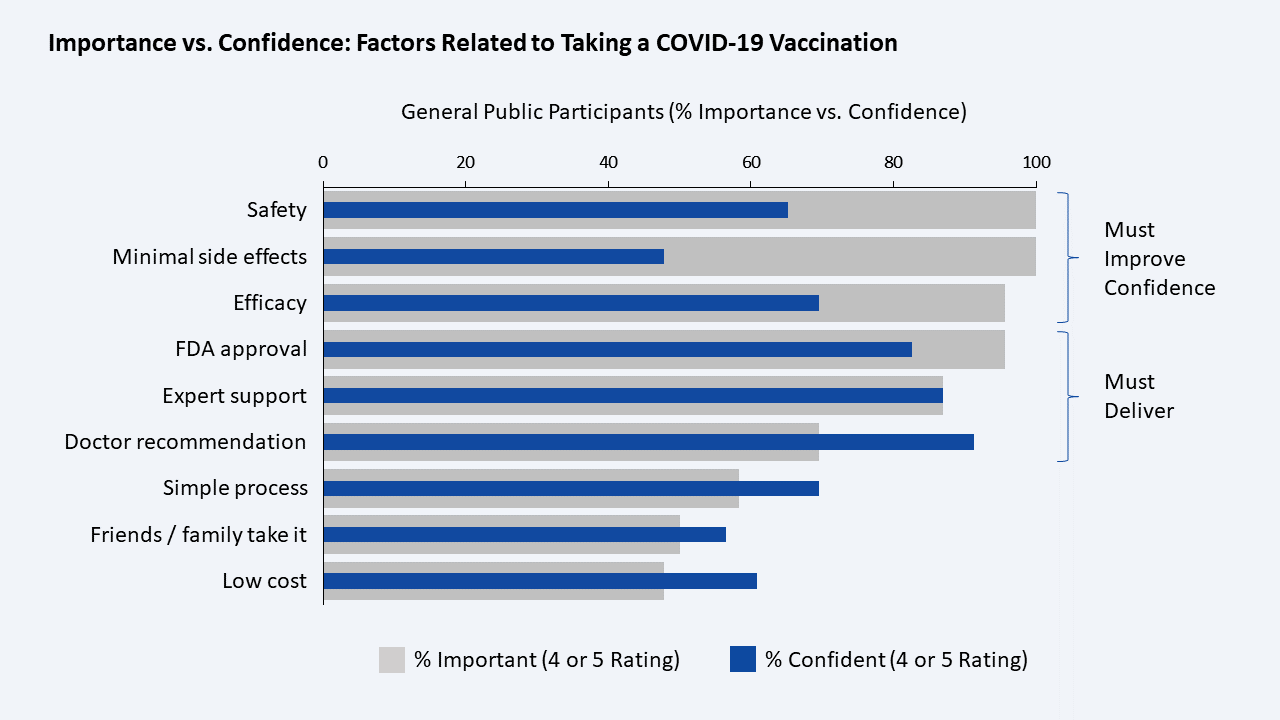
Finding: There are large gaps in overall confidence in the most important factors for taking a COVID-19 vaccine. 83 percent are confident that a vaccine will be approved by the FDA, 70 percent that it will be effective, 65 percent that it will be safe, and only 48 percent that it will have minimal side effects. There is a significant difference in the degree of confidence between those who are likely to take the vaccine and those who are not, with the latter group much less confident of vaccine safety (36 percent versus 92 percent) and minimal side effects (18 percent versus 75 percent).
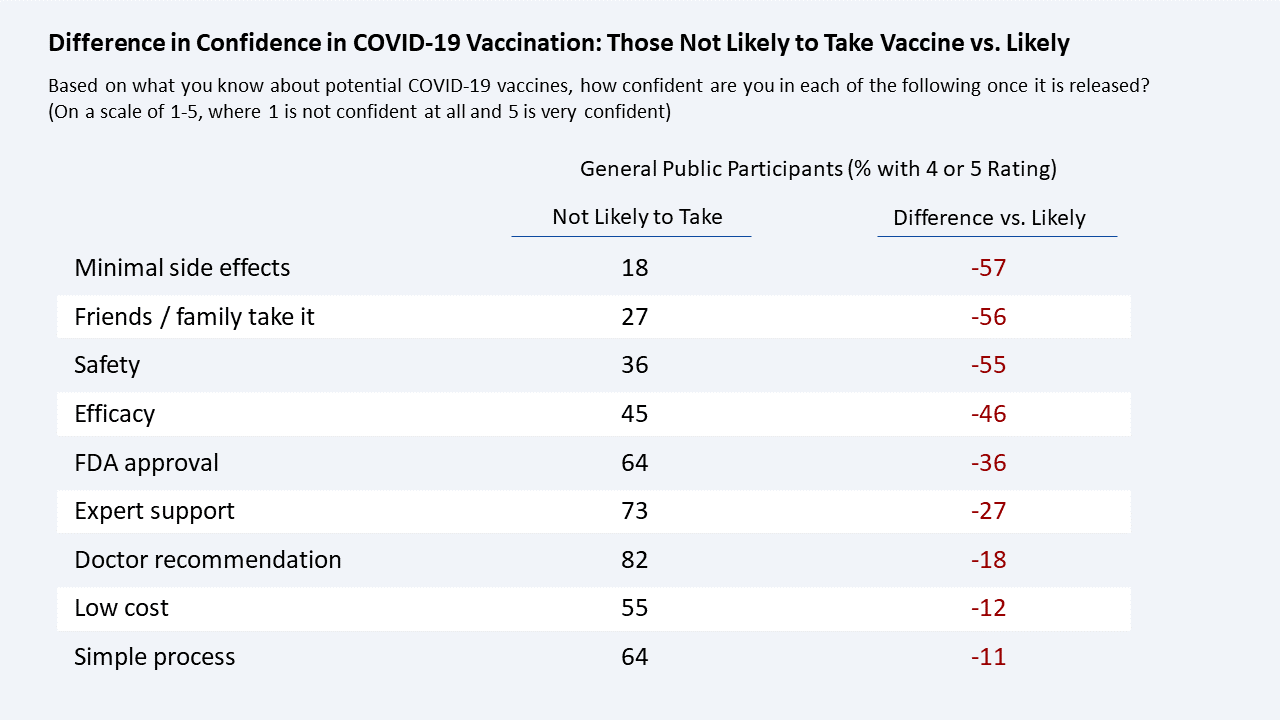
Why This is Important: The two most important factors – safety and minimal side effects – have some of the lowest levels of public confidence, driven down by those who are not likely to take the vaccine. There is a strong “wait and see” attitude: participants want to see evidence that the vaccine works on others outside the trials. “I would want to make sure that it doesn’t have any horrible side effects. I wouldn’t want to be one of the first to take it. I want to make sure it’s been tested,” said K., a research technologist from Santa Fe, New Mexico.
Implications: We mapped participants’ rated factors to show the relative level of importance and the confidence for each factor. We identified the areas that are “must deliver,” factors that are both important and inspire high confidence. We also identified the areas that are “must improve confidence,” factors that are important and lagging in confidence. The “must deliver” areas are already assumed to be true and thus already baked into the cake. An effort to ensure that these come to fruition is critical. In addition, expectations for some of the less important items with high confidence (FDA approval, expert support, and doctor recommendation) must be fulfilled through health experts publicly communicating trust in a vaccine and doctors advocating for it. The “must improve confidence” areas require targeted initiatives that strengthen the public’s faith. These are the factors (safety, minimal side effects, efficacy) that will require the biggest effort and have the most leverage to improve adoption rates.
Women Are Household Gatekeepers:
Finding: Women in our study were more likely to be the primary health decision makers for multi-person households. 75 percent of women who live with others said that they make decisions related to health for the household, compared with 25 percent of men who live with others.
Why This is Important: It is always good to know who the decision makers are when trying to alter behavior. Not only are women more influential in the household, but women making household health decisions are also less likely to take a COVID-19 vaccine themselves (33 percent versus 50 percent for men). This difference is consistent with other studies showing a 20-point gender gap.
Implications: It is important to address the specific concerns of women, who have historically been largely ignored both in terms of clinical trial participation and input into the development of drugs. It is not sufficient to have a one-size-fits-all approach to increasing trust in new vaccines. Women should be placed in larger leadership roles in vaccination development and distribution processes, and more input from women should be incorporated into planning.
Doctors and Nurses Are Not on Board Yet:
Finding: Only 59 percent of doctors and nurses say that they are likely to take the vaccine. Dr. R., a physician from Atlanta, Georgia, expressed reluctance: “I’m not running out to be the first one in line to get it. I’ll only get it early if it’s mandatory to get it as a doctor.”
Why This is Important: This is an alarmingly low figure. One of the groups that the vaccine will be available to earlier than others is frontline medical workers. If many of them opt out of taking it, it sends a negative signal to others who value their opinion. Health providers are more likely to recommend the vaccine for their patients, especially those in the COVID “high risk” category.
Implications: There should be a stronger effort to gain the support of the broader medical community. The good news is that a higher percentage (71 percent) of the doctors and nurses we spoke with indicated that they plan to recommend the vaccine to at least some of their patients. This still leaves room for improvement, especially given that a doctor’s recommendation is an important factor for many Americans.

There is Skepticism of Institutional Medicine:
Finding: Overall, 70 percent of the general public participants indicated that a recommendation to take a COVID-19 vaccine from their doctor was an important part of their decision calculus. However, only 45 percent of those who do not want to take the vaccine said a doctor’s recommendation was important.
Why This is Important: This is about half the level of the 92 percent of those who plan to take the vaccine, who prioritize their doctor’s recommendation. This is further complicated by the fact that there is heavy skepticism concerning vaccines in general. Last year, the WHO listed vaccine hesitancy as a top ten threat to global health. Dr. K., a psychiatrist from El Cerrito, CA, noted, “Previously, I never thought much about it. But with COVID I’m more concerned because it’s been pushed through quickly.” People are trading off risks, and many believe the risk of a vaccine outweighs the risk of getting coronavirus.
Implications: The mumps vaccine was developed in a record four-year period ending in 1967. It is understandable why many are more worried about the fast pace of COVID-19 vaccine development. It is incumbent upon our leaders to explain in clear terms why these new vaccines, created at breakneck speeds, will be reliable. We found that there is a “worry gap,” a split between people who were worried about getting COVID-19 among people who are likely to take the vaccine and those who are not. 64 percent of those who are worried about getting the virus are likely to take the vaccine, while only 33 percent of those who are not worried of it plan to take the vaccine. This worry gap can be addressed through better messaging and building a stronger sense of trust in institutional medicine.

Biden’s Win Improved Adoption:
Finding: We asked participants about their political and policy views, including who they voted for in the recent presidential election. We also asked how President-Elect Joe Biden’s management of vaccine distribution will impact the likelihood that participants will take the vaccine. Those who voted for President Donald Trump said that they were unaffected by Biden taking on the leadership role of distribution. However, 53 percent of Biden voters in the general public group (and 55 percent of the medical professional group) said that Biden’s forthcoming oversight of distribution makes them more likely to take it.
Why This is Important: The pandemic has been politicized in many ways, from state shutdowns to masks, and the vaccine, too, has fallen victim to polarization. V., a resident of Knoxville, Tennessee, is at high risk for COVID-19 due to severe asthma. She said, “Biden is going to follow what the scientists’ recommendation are. The other one would fast track it for political reasons where it may not be as safe.” Biden’s forthcoming presidency late next month gives people one less reason to avoid taking it.
Implications: Joe Biden’s victory had a net positive impact on vaccination adoption. If Democrats continue to be more optimistic and Republicans do not lose confidence, more people will get vaccinated. It is important for Biden and his administration to be transparent and direct with the American people to avoid erosion of confidence in the vaccine among his political detractors.
“It makes sense for me. I’m older and I have a low immune system.”
– W., a retired 74-year-old from Port St. Lucie, Florida
Large Variation Among Certain Demographic Groups:
Finding: We noted the gender gap earlier. Although the study’s sample is too small to make conclusive statements about differences between smaller demographic segments, we found trends consistent with other studies and heard comments supporting the data. Across many groups, we see large differences in likelihood of taking a COVID-19 vaccine. Black and Latino participants in our study were less likely to say they will get vaccinated (38 percent versus 57 percent for other races), consistent with a recent study showing a racial difference attributed to mistrust. “Typically, African Americans have been used as guinea pigs. Also, I want to make sure it has been sufficiently tested on the African American population,” said S., a stay-at-home mom from Ladson, South Carolina. In Tuskegee, Alabama, syphilis medication was withheld for forty years from a group of African Americans, without their knowledge, as part of a sinister study funded by the U.S. Public Health Service. Participants over the age of 50 are much more likely to take the vaccine, at 80 percent likely compared with 44 percent likely for those 50 and under. W., a retired 74-year-old from Port St. Lucie, Florida, said, “It makes sense for me. I’m older and I have a low immune system.” We observed a similar correlation for those in high risk groups. Furthermore, doctors and nurses said they were much more likely to recommend a COVID-19 vaccine to those at increased risk.
Why This is Important: This data indicates that there are gaps not only in certain categories of vaccine performance, but also – due to demographic differences – in the willingness to take it. Knowledge of these demographic differences is helpful for our policymakers to determine where and how to invest.
Implications: Clearly, a lot of work needs to be done to prove to Black and Latino Americans that their well-being will be taken into consideration in the development of the vaccine. The CDC plans to prioritize several groups, including “people at high risk for severe COVID-19 illness due to underlying medical conditions” and those aged 65 and older. It is encouraging that participants in these groups are likely to take the vaccine.
Although we clearly have an uphill battle to increase COVID-19 vaccination adoption, history gives us reason for optimism. When the polio vaccine was released to the general public, only 60 percent of Americans said they would take it. Eventually, adoption rates were much higher, and the U.S. has been polio-free for decades ever since. We can eradicate this coronavirus as well, but it will require our leaders, policy makers, and health experts to exert significant efforts to ensure that it happens as soon as possible.
HOW THE STUDY WAS CONDUCTED
Avenue Group conducted confidential one-on-one interviews over the phone between November 13-23, 2020, during a surge in coronavirus cases across the U.S., and, after President-elect Joe Biden had been declared the winner of the presidential election. Average interview length was 30 minutes. Participants did not know the specific interview topics prior to our scheduled interviews. Participants responded to a request for an interview about health and personal views. They shared their personal perspectives on COVID-19-related issues across health, finances, family, and politics. Participants comprised a representative sample of American society, across gender, race, income, geography, employment status (medical provider, essential worker, non-essential worker, not employed, unemployed), level of education, political affiliation, and other demographic factors. 52 percent of participants know someone who has been hospitalized for COVID-19 and 39 percent know someone who has died from the virus.
To discuss our findings or learn more about the study, please contact us.






Leave a Comment